
Introduction
Located one mile north of downtown Las Vegas and two blocks south of the city’s homeless shelters, Vegas Stronger is a non-profit organization focused on reducing our city’s homeless population through substance-abuse treatment. Almost 6,000 citizens of Las Vegas are homeless1 and 3,000 of those are unsheltered. Internal studies report almost 90% suffer from a substance-abuse disorder. Our goal is to offer treatment to every single one of these individuals in 2023 with the same quality one would receive at a for-profit institution located in a high-income area. We partner with both NGO’s and government agencies throughout the city to provide housing to ensure those who enroll at Vegas Stronger for treatment have a place to live. We also partner with other medical facilities throughout the city to provide treatment outside of our level of care. We have served over 300 clients since we began in the summer of 2020, and in 2021 we moved into a renovated facility boasting a boxing gym, salon, gift shop, and group treatment rooms.
This study is done in part to determine the efficacy of the Vegas Stronger Thirteen Elements (see Section 3) treatment method, and in part to refine our program to best suit the needs of our clients. As a young organization, it is important to improve our treatment program while systematic change within the company is relatively easy. While reading, please understand it is difficult to obtain any concrete conclusions based on these preliminary data. I reserve the right to make any changes to this report based on any new and evolving information.
1)shorturl.at/hnRUX
13 Elements of Vegas Stronger
Counseling and Psychiatric Treatment
Vegas Stronger currently offers four modes of group treatment of Level I and Level II services: Outpatient Program (OP), Partial Hospitalization Program (PHP), Mental Health, and Intensive Outpatient Program (IOP). All of our programs are designed for clients who do not require medical detox or around-the-clock supervision. Our clients are assigned to groups based on the severity of their diagnosis. Clients in our PHP program meet in groups for nineteen hours per week; clients in our OP program only meet for one hour a week (along with individual sessions.) Clients in our mental health group work with a clinician for 9 hours a week; this program is designed for those suffering from clinically diagnosed mental health issues as well as substance abuse.
Most of our clients are currently enrolled in our IOP program, meeting three times per week for three hours per session. Based on clinician opinion, clients usually complete the program after four-to-six months of group attendance and participation. This report is based on results gathered from IOP clients.
IOPs are the second-most common treatment program for substance abuse disorders behind regular outpatient treatment. There is significant evidence across the literature regarding the effectiveness of IOP in alleviating substance-use disorders. A meta-analysis of twelve studies found IOPs are as effective as inpatient treatments when studies compare these approaches. (McCarty, et. al., 2014) IOPs represent a higher level of care than usual outpatient services and a lower level of care than inpatient services. They provide treatment for symptoms associated with substance-use disorders. Outside of group counseling, IOP groups typically provide individual counseling, psychoeducational programming, the monitoring of drug and alcohol use, case management, medical treatment, and psychotherapy. (SAMHSA) These are all intended to help the client learn relapse management and prevention, develop coping strategies, and improve well-being. At Vegas Stronger our clinicians utilize methods such as motivational interviewing and psychotherapy in our IOP groups.
Case Management
Ziguras and Stewart (2000), in a meta-analysis of 35 studies with a total of over 6,000 patients, found case management during treatment leads to lower dropout rates and improvement in social functioning. Case managers are a liaison between clients, the community, and health care professionals to improve treatment. Case managers at Vegas Stronger work with our clients to find housing, primary medical care, employment, and resolve any other issue that would increase the likelihood of long-term sobriety. At Vegas Stronger, our case managers help our clients meet outside health needs, enroll them in health care benefits (e.g., insurance), and provide them with basic necessities. All of these services are tailored to the individual client to ensure they are receiving the highest level of care we can provide. Our case managers improve the lives of our clients, the treatment they are receiving, and the lives of everyone in the client’s milieu (including Vegas Stronger employees). Vegas Stronger currently employs two full time case workers, with a plan to expand to six in 2023.
Medication Assisted Treatment
Medication-assisted treatment (MAT) is the use of FDA-approved medications to aid the client in recovery. At Vegas Stronger, we offer naltrexone and buprenorphine. Used in combination with counseling and behavioral therapies, these can vastly improve the outcomes of our clients. All our prescribed medications are clinically driven and tailored to meet each patient’s needs. All of the medications we offer are evidence-based treatment options.
Primarily, MAT is used for the treatment of addiction to opioids. These medications alter brain chemistry while blocking the euphoric effect of substances. Depending on the medication, they can relieve physiological cravings as well. MAT has been shown throughout the literature to sustain and prolong recovery. The use of medications combined with treatment is superior to either used on its own. (American Society of Addiction Medicine) MAT can prolong treatment duration and reduces the likelihood of relapse. (Mattick, et. al., 2009)
At Vegas Stronger we offer buprenorphine to treat opioid-use disorders and naltrexone to treat both alcohol- and opioid-use disorders. Buprenorphine is a partial agonist – it binds to the body’s opioid receptors, partially blocking the euphoric effects of opioids and alleviating withdrawal symptoms. Naltrexone is an antagonist – it covers the body’s receptors, blocking the effects of opioids if they are used. We also distribute NARCAN (naloxone) to our clients to prevent opioid overdose by reversing the toxic effects of the overdose.
Drug Testing
At Vegas Stronger we drug test our clients (via urinalysis) randomly at least once a week, based on clinician opinion. Drug tests are used throughout our treatment process for a variety of reasons. First, we use drug tests during the client’s Biopsychosocial preliminary examination to determine if there are any drugs in the client’s system so they can be sent to medical detoxification (if necessary) and determine the appropriate level of care.
We realize those suffering from substance-abuse disorders may not be entirely honest when entering our program. They also may be in a state where they do not know or remember which substances they have consumed. It is especially important to know what drugs are in the client’s system before prescribing any medication assisted treatment medications, as they may interact with the substances in the client’s system, resulting in serious side effects.
When these random drug tests will occur is difficult for the client to predict and can prevent relapse while in treatment. They can facilitate a lifestyle free from harmful substances. We currently contract with a medical provider to drug-test our IOP clients at least once a week; as clients “step down” to lower levels of care these drug tests become less frequent.
Primary Medical Care
A majority of our clients do not have access to primary medical care upon admission. As many of them are homeless, they have not seen a physician for a significant period of time. Obtaining primary medical care for our clients while in treatment provides benefits to both the patients and the clinicians. By being healthy, our clients can better focus on recovery and interpret the messages they receive from their clinicians in group. Samet, et. al. (1996) show patients who receive primary medical care while in substance-abuse treatment are less likely to relapse A similar study shows patients also have better overall health and provides structure. (Samet, et. al., 2001) Our case managers work with the client’s insurance provider (usually Medicaid) to find a primary care physician for all those without.
Housing
Stable housing is perhaps the most important part of recovery. Having a roof over your head each night provides structure and can make the recovery process easier, and alleviates the need to “cope” with alcohol or drugs. (Johnson, 2007) Sinha (2018) notes the stress of not having housing can increase the likelihood of relapse. Vegas Stronger works with community providers (both NGO’s and government agencies) to provide housing for all our clients within one week of admittance. (As our program is contingency-based, we only provide housing to patients enrolled at Vegas Stronger.)
Spirituality
The role of spirituality is helpful in aiding recovery from substance-use disorders. Per Lyons, et. al., (2010), 82% patients who focused on their spirituality were substance-free at the twelve-month mark, versus 55% of those who did not. Grim and Grim (2019), in a meta-analysis, cite 84% of studies show belief in a higher power promotes relapse and prevention. Spirituality has been shown to help clients find renewed purpose, promote accountability, connect them with something outside themselves, increase compassion and humility, and promote greater mindfulness. (n.d.)
Peer Recovery Coaching
Peer recovery support is the giving of non-clinical assistance to support clients in recovery. Relatively new to treatment programs, this support now plays an important role in a holistic treatment program. Peer recovery coaches have attained long-term sobriety and are professionally licensed. Peer recovery specialists also help clients accumulate the resources necessary to maintain recovery. (Best & Laudet, 2010; Coud & Granfield, 2008). White (2009) notes they can help initiate and maintain recovery by enhancing the quality of life of the patient. Vegas Stronger currently employs two full-time recovery coaches, and will expand this number in 2023.
Recovery Meetings
Donovan, et. al. (2013) synthesize the vast literature regarding the positive relationship between 12-step recovery meetings and long-term sobriety. Participation in AA and NA is associated with a greater likelihood of abstinence (Humphreys, et al., 2004; Krentzman et al., 2010) for up to 16 years (Moos & Moos, 2006). These studies also show mental and emotional functioning. Donovan et al. also cite that regular meeting attendance while in treatment (moreso if the meetings are held at the facility location are associated with improved psychological outcomes, and attending meetings at least three times a week results in better substance use outcomes. (Although they do note this may be a result of outside factors of attendance, e.g., service work, step work, or getting a sponsor.) Other studies show that remaining in 12-step groups after completing treatment is beneficial as well (Humphreys & Moos, 2001, 2007).
Donovan et al. also cite studies showing a higher level of causality beyond simple correlations. Recent studies using advanced econometrics refute outside influence such as participant quality, level of motivation, or severity of the clients’ substance-use disorder. These analyses provide more evidence that 12-step meetings play a vital role in a treatment program. (Connors, Tonigan, Miller, & Project MATCH Research Group, 2001; Kaskutas, 2009; Krentzman et al., 2010; McKellar, Stewart, & Humphreys, 2003; Weiss et al., 2005)
Our clients are encouraged by our clinicians to attend 12-step meetings while in treatment, and we host NA meetings in our facility every day of the week.
Salon Services / Fitness and Yoga / Nutritional Services
Having a negative body image can lead to drug and alcohol abuse. (Specter and Wiss, 2014) A survey of the literature by Smith and Lynch (2012) reveal individuals who engage in regular aerobic exercise are less likely to use and abuse illicit drugs. Exercise reduces the likelihood of relapse through several behavioral and neurobiological consequences of exercise in all phases of recovery. To improve our clients’ self-perception and reduce relapse potential, we offer salon and fitness services. Volunteers from the community visit our facility biweekly to provide free salon services to our clients and our gym is available for use six days a week. We employ two trainers on staff to lead boxing and general fitness classes, and also offer yoga classes three times a week.
Service to Others
One of the more common sayings one may hear at an AA meeting is “You have to give it away to keep it.” Service is a tenet of any recovery group. Through service to others, one can remember where they came from, and are less likely to return. They are also likely to have higher self-esteem and suffer less from depression.
Data and Results
Six-Month Follow-Up
From June 2021 to May 2022, Vegas Stronger accepted 141 unique clients into its IOP program. All of these clients were administered an introductory survey regarding housing, employment, drug history, and demographics (partially as a requirement to maintain accreditation through the monthly submission to the Treatment Episode Data Set). Six months post-admission, Vegas Stronger attempted to follow up with these clients – of which 29 clients completed (20.6% completion rate).2 Unsurprisingly, the majority of those who completed a follow-up survey completed from IOP and sustained a length of stay typical of a full IOP program. At the six-month follow-up survey, we ask our clients a variety of questions to determine their sobriety (via urinalysis testing), employment status, housing status, and well-being using the Rating of Outcome Scale (ROS). (The ROS is a widely-used, evidence-based tool to determine the mental and emotional state of the interviewee. 3)
2) Twelve-month follow-up surveys have also been completed, however the sample size is minimal and unworthy of being included in this analysis.
3) https://www.thecoloradocenter.com/dev/Seideletal2016PreliminaryValidationPsychAssess.pdf
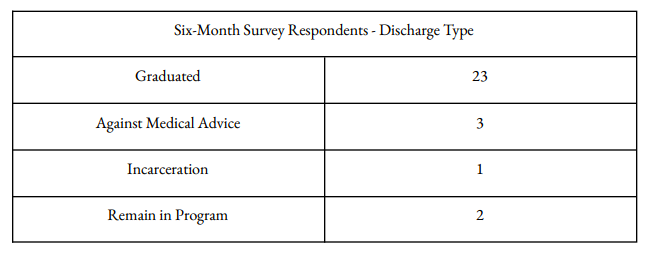
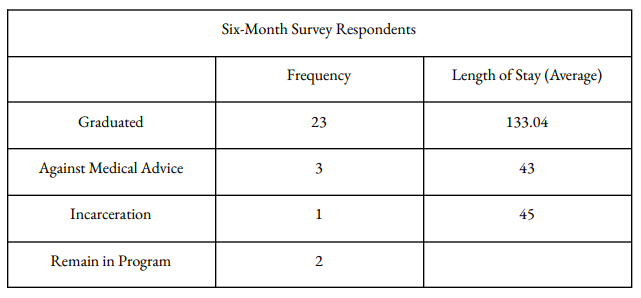
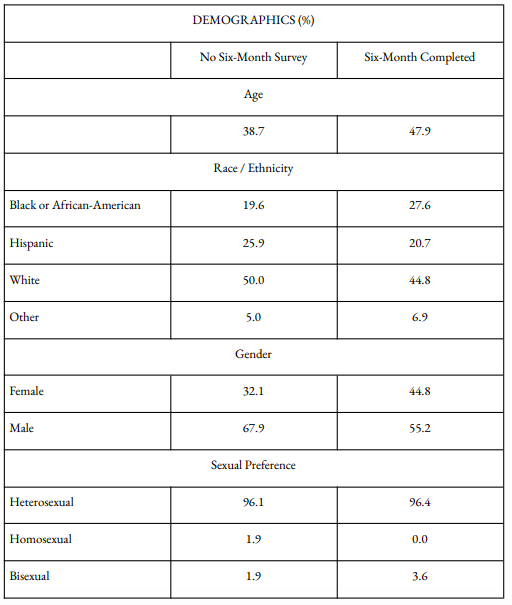
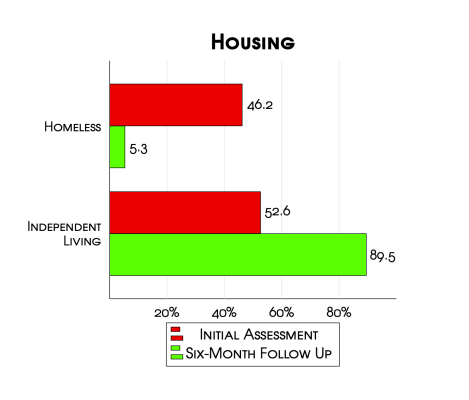
Clients who complete a six-month follow-up survey are more likely to be female and older. However outside of gender, age, and reasons for discharge, clients who completed a six-month survey differ little from the entire 141-client sample in terms of demographics, housing4, employment, and wellbeing. (The variance that does exist reveals clients who completed the follow-up survey – a majority of whom graduated – had lower levels of employment and less stable housing when entering the program, perhaps giving credence to the “rock-bottom” thesis.)
4) Those incarcerated before beginning treatment at Vegas Stronger are not listed in the chart.
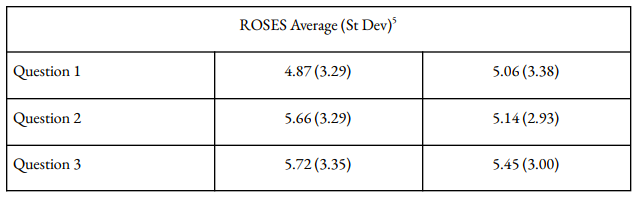
5) The differences in results are statistically insignificant across the questions. Respectively, t-values are 0.22, 0.62, and 0.33 from two-tailed difference of means tests.
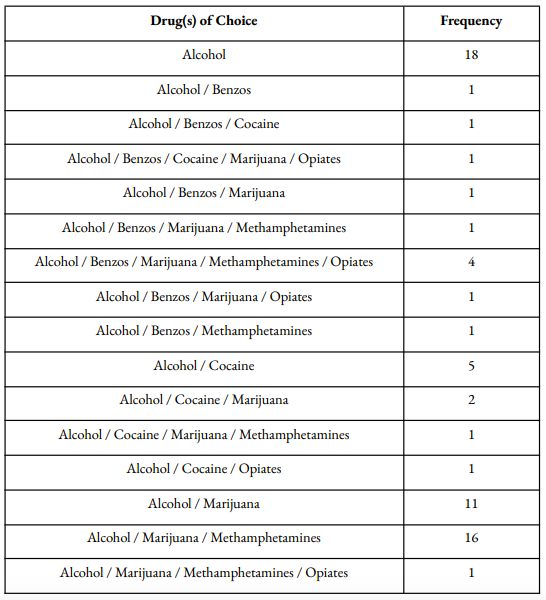
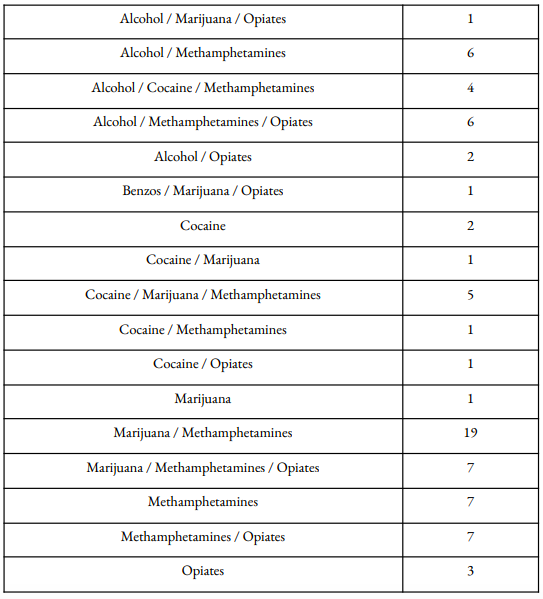
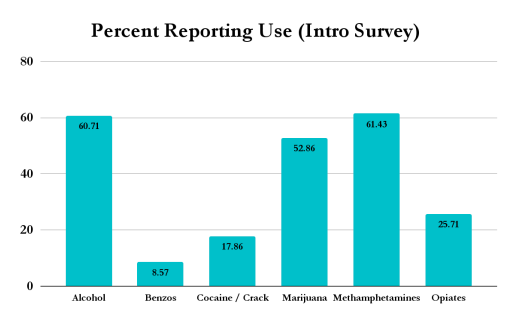
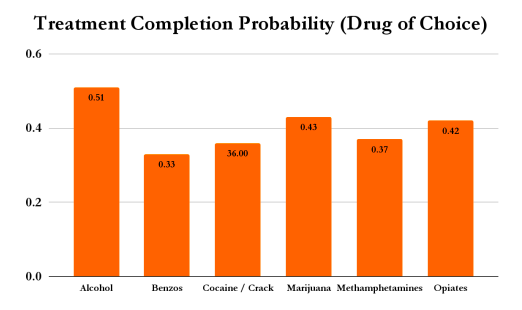
The most popular drug of choice for Vegas Stronger clients is methamphetamines, followed by alcohol. Out of all clients, 110 (78.0%) have co-occurring disorders. Our clients who report alcohol as a drug of choice are most likely to complete IOP treatment, and reported use of benzodiazepines results in the lowest probability of treatment completion.
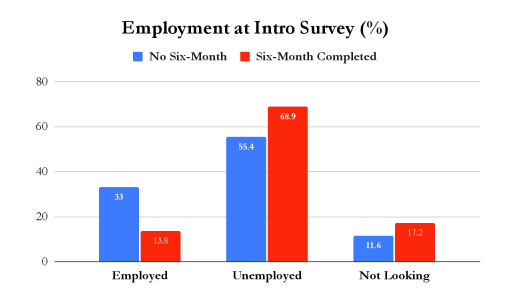
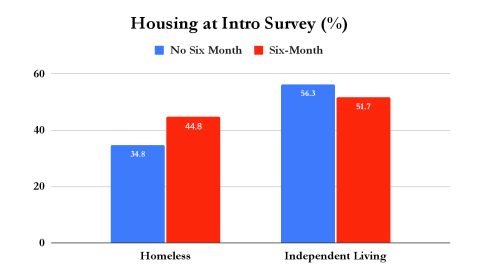
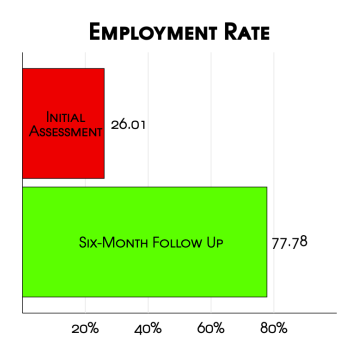
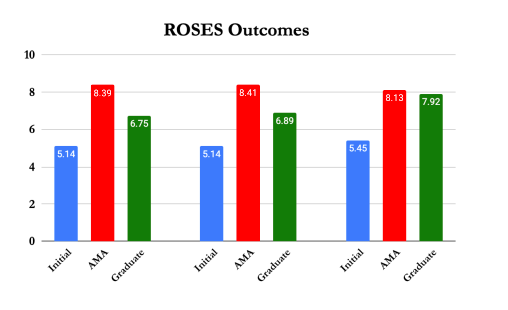
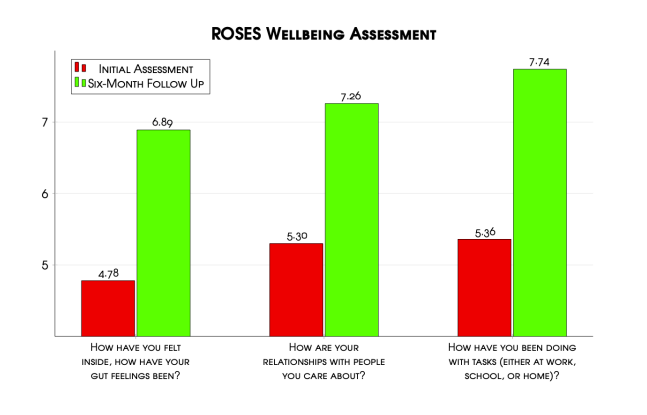
Preliminary analysis reveals our clients see vast improvements across our four outcome measures from their initial interview to the six-month follow up. Across all clients, 63% are free from substance-use at six months. For those who complete treatment, that number jumps to 83%. We also see significant improvements in housing, employment, and well-being. While our clients who leave before completing treatment (AMA – Against Medical Advice) see more improvement across the well-being metric than those who complete treatment, this is likely due to the limited sample size mentioned previously.
Weekly Surveys
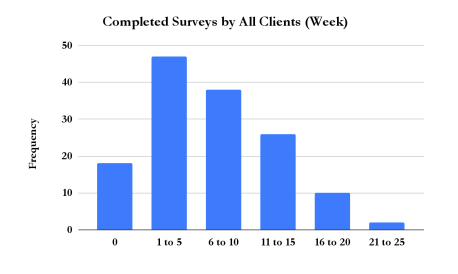
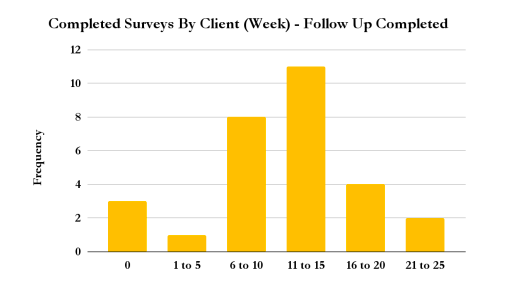
Each week, all Vegas Stronger clients are asked to complete a survey based on their participation in the Thirteen Elements of the Vegas Stronger Method which we offered at the time the survey was administered.6 All admitted clients in the aforementioned time frame completed a total of 966 weekly surveys, while the 29 clients in the follow-up sample completed a total of 323 (ranging from zero to twenty-two). The surveys are categorized by the week of attendance in which the client completed it. (As the questions refer to participation in the Thirteen Elements in the previous week, any survey completed before the seventh day of enrollment is categorized as Week 0.) The charts below which contain “Week” on the x-axis refer to the week of survey completion by the client. The survey is included in the appendix. In each subsection I include summary statistics for each of the offered Thirteen Elements, as well as conditional probabilities for each of the four outcome measures based on their weekly answers. Unless noted, the charts refer to the weekly surveyed completed by only those who completed a six-month follow up survey. Not all of the thirteen elements are included here. Five of them (nutritional services, medication-assisted treatment, primary medical care, and peer recovery coaching) were either not offered to these clients (due to lack of resources) or unable to be properly tracked.
6) The survey is included in the appendix.
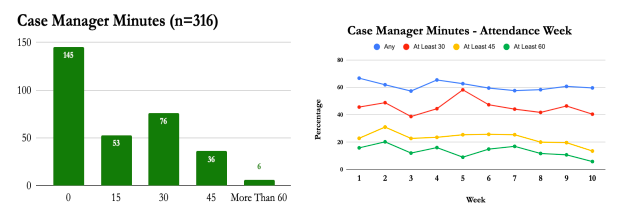
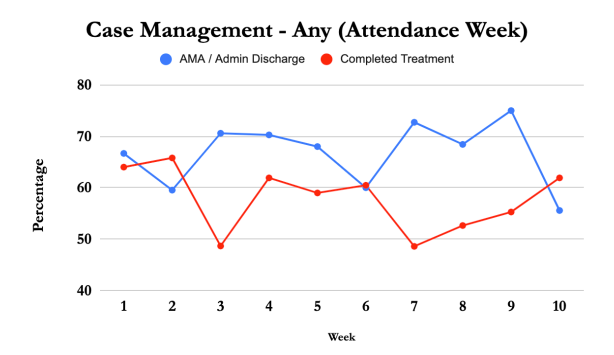
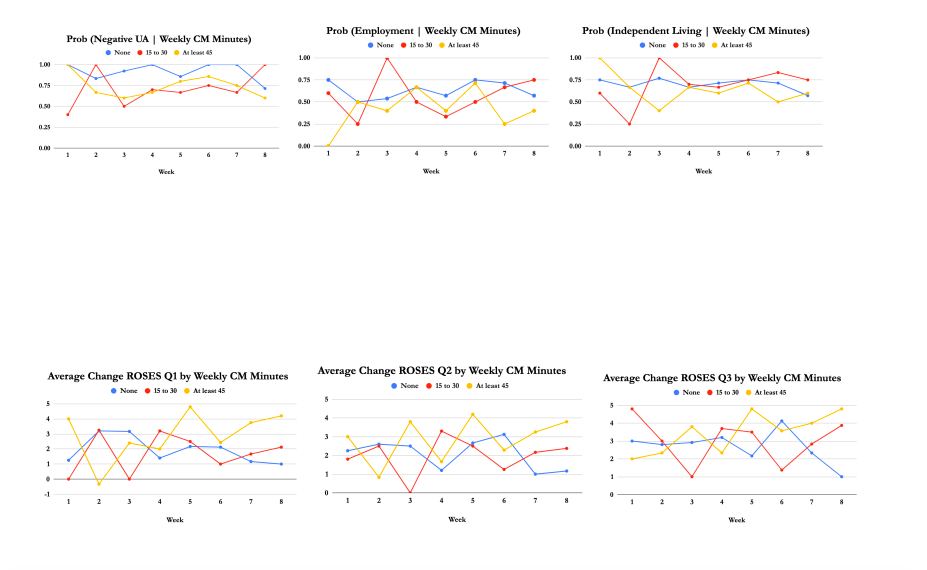
Case Management
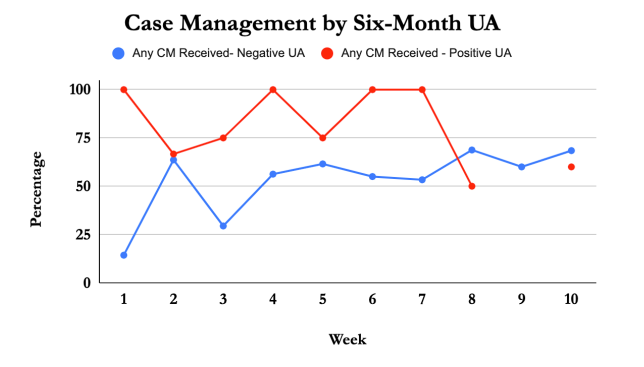
Vegas Stronger clients received on average 22.48 minutes of case management each week. Those who completed IOP received 19.81 minutes per week, compared to 28.26 for those discharged prematurely. As those who suffer the most from a substance-use disorder require the most case management, it is unsurprising those who receive more case management are less likely to complete treatment, as those suffering most from their substance-use disorder require the most care. For example, a higher percentage of clients who receive any Case Management throughout their tenure at Vegas Stronger test positive for substances at six months for Week 1-7.
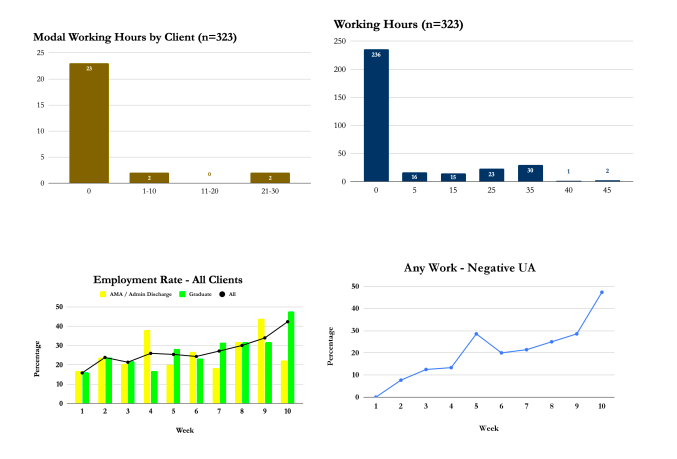
Employment (Any Working Hours)
We recommend to our clients to refrain from working in their first few weeks of enrollment in order to focus on their recovery. However as they become more stable, we realize employment is a necessary step to refraining from substance-use moving forward. As a result, most of our clients do not work while in treatment, however a greater percentage of our clients find employment as their tenure increases. Almost all of our clients are unemployed when entering our program. But while enrolled at Vegas Stronger, 36% of them find work (ranging from beginning employment from Week 2 to 16.) It is inconclusive as to whether working while in treatment has any effect on any of the outcome measures. Although (tautologically), working while in treatment does increase the likelihood of working six-months post-admission.
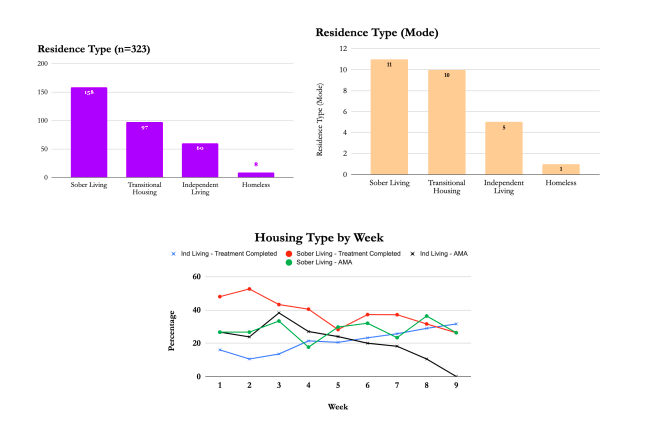
Housing
One of the first steps in serving our homeless population is giving them a place to live outside of the local shelters. This usually means residence in a transitional housing facility (e.g., Crossroads) or with one of our partners in a sober living home. Very few of our clients live independently upon admission, so our case managers work with almost all our clients with regards to their residency. Those who live in sober living homes are more likely to have a negative UA test at six months, however those living in transitional living see higher increases in their well-being.
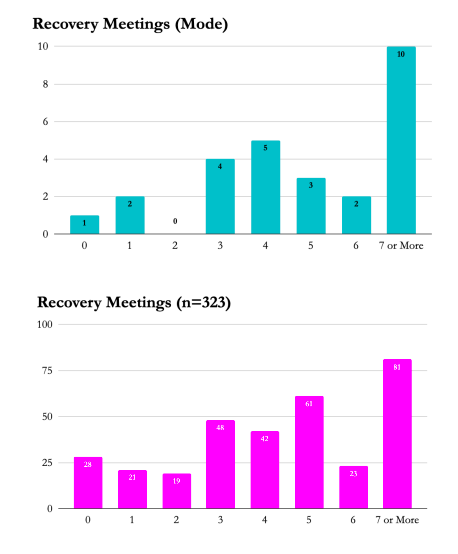
Meeting Attendance
We believe encouraging our clients to attend either Alcoholics Anonymous or Narcotics Anonymous meetings is essential to the recovery process. Obtaining a sponsor and attending daily support groups (outside of groups at Vegas Stronger) helps build an infrastructure to maintain life-long sobriety. It is unsurprising that those who attend AA or NA meetings have better emotional outcomes across all measures than those who do not. Thus far, it is inconclusive as to the effect of meeting attendance on other outcomes.
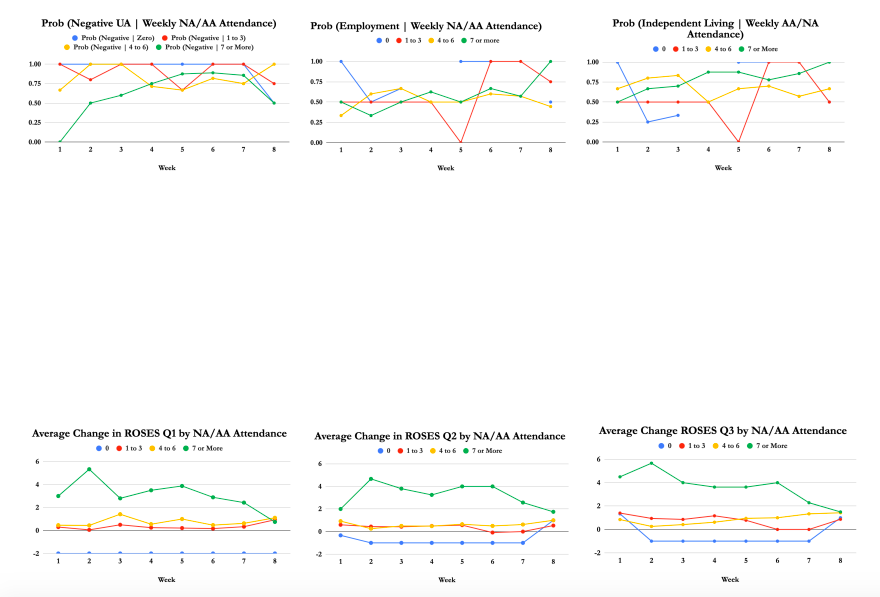
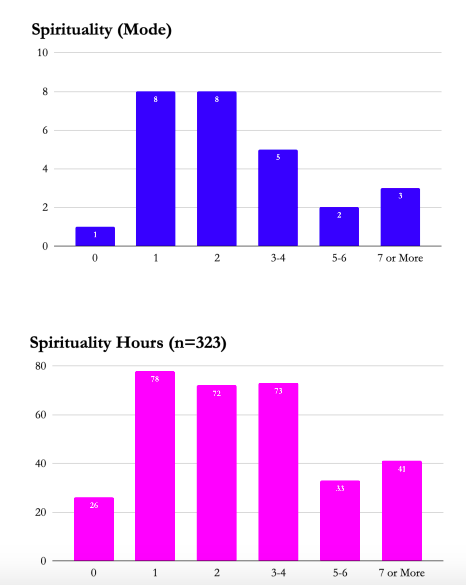
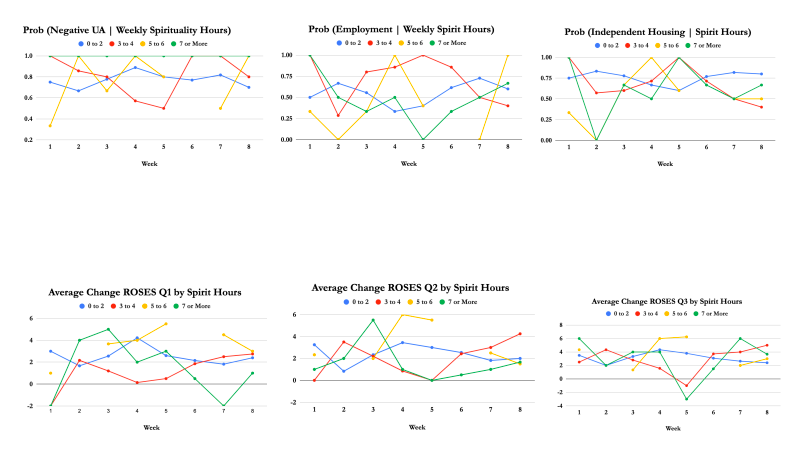
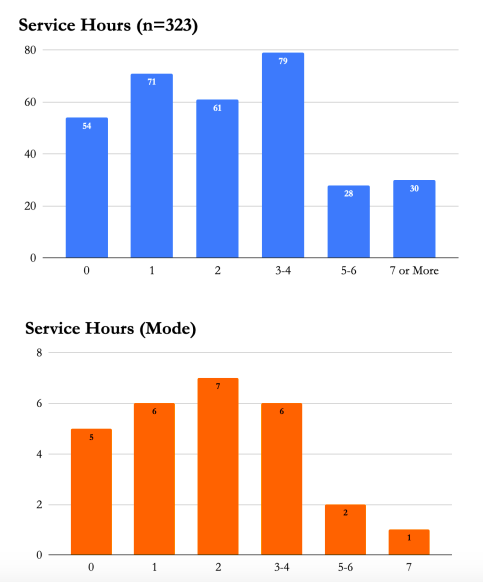
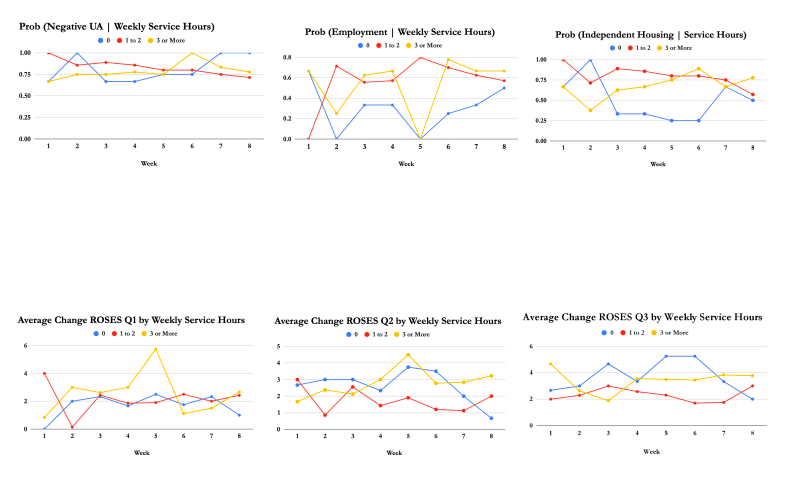
Spirituality
Our clinicians encourage our clients to make daily contact with their higher power, no matter what He, She, or It may be. Our clients who spend at least one hour a day working on their spirituality have a 100% likelihood of attaining sobriety six months post-admission.
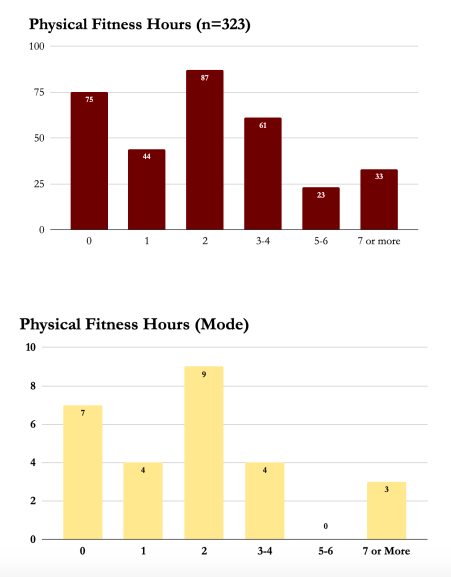
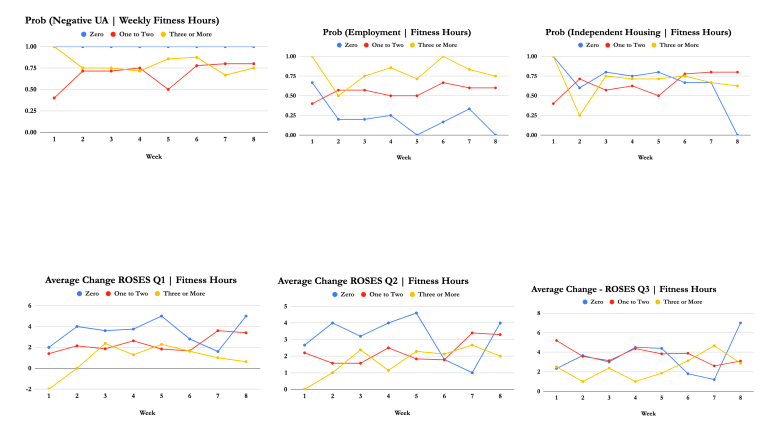
Fitness
We also believe daily exercise is important. Attaining the high one gets from dopamine and serotonin release through breaking a sweat (and making the body feel good) is essential in the recovery process. However those who never exercise have a 100% likelihood of having a negative UA. So who knows, really. But those who exercise are more likely to be employed at six months.
Salon Services
You look good, you feel good. That is the basis for offering a biweekly salon in our building, free of use to our clients. Of the 27 clients who completed a follow-up survey, 19 of them (70.3%) received salon services while at Vegas Stronger, and 8 of 27 (29.6%) received salon services at least once every six weeks. Of the clients who received a salon visit, fifteen of them reported a negative UA test. Fourteen lived independently, and fifteen of the nineteen were employed.
Service
Understanding you are not alone in recovery is essential. And the best way to do that is to serve others realizing the world is bigger than yourself, and letting go of selfish thoughts, is key to maintaining sobriety and becoming a productive member of society.
Conclusion
While current results are preliminary, there is some evidence about the effectiveness of the Vegas Stronger treatment method (notably, the importance of service and meeting attendance on the four aforementioned outcomes).
Many studies have determined the singular effect of each of our Thirteen Elements on client outcomes, however there are yet to be any analyses studying the combined effect of each of these elements together. While the goal of completing this analysis is ambitious and challenging, it is possible with the further collection of data and refinement of measurement methods. Advanced econometric techniques have provided the tools to perform this analysis, however to determine any positive causality (if it exists) throughout the elements together, we need significantly more data (and therefore, a significantly larger client base). We have already expanded our services to include Medication Assisted Treatment, but it is not analyzed here as none of the clients in the sample were on it at the time of their treatment. We also have added biweekly salon service available to our clients (at no cost, of course).
It is also our hope to expand our census significantly in 2023 (as well as geographic expansion in Reno and Pahrump), therefore increasing the sample size and allowing better econometric methods. This also provides more contrast in the data, as those in Reno and Pahrump will not have the same set of services available to them as those clients in Las Vegas.
References
American Society of Addiction Medicine, The ASAM National Practice Guideline.
Best, D., & Laudet, A. (2010). The potential of recovery capital. London: RSA.
Cloud, W., & Granfield, R. (2008). Conceptualizing recovery capital: Expansion of a theoretical
construct. Substance use & misuse, 43(12-13), 1971-1986.
Connors GJ, Tonigan JS, Miller WR Project MATCH Research Group. A longitudinal model of
intake symptomatology, AA participation and outcome: Retrospective study of the Project MATCH
outpatient and aftercare samples. Journal of Studies on Alcohol. 2001;62(6):817–825.
Donovan DM, Ingalsbe MH, Benbow J, Daley DC. 12-step interventions and mutual support
programs for substance use disorders: an overview. Soc Work Public Health. 2013;28(3-4):313-32. doi:
10.1080/19371918.2013.774663. PMID: 23731422; PMCID: PMC3753023.
Grim BJ, Grim ME. Belief, Behavior, and Belonging: How Faith is Indispensable in Preventing and
Recovering from Substance Abuse. J Relig Health. 2019 Oct;58(5):1713-1750.
Humphreys K, Moos R. Can encouraging substance abuse patients to participate in self-help groups
reduce demand for health care? Alcoholism: Clinical and Experimental Research. 2001;25(5):711–716.
Humphreys K, Moos RH. Encouraging posttreatment self-help group involvement to reduce demand
for continuing care services: Two-year clinical and utilization outcomes. Alcoholism: Clinical &
Experimental Research. 2007;31(1):64–68.
Humphreys K, Wing S, McCarty D, Chappel J, Gallant L, Haberle B, Weiss R. Self-help organizations
for alcohol and drug problems: Toward evidence-based practice and policy. Journal of Substance Abuse
Treatment. 2004;26(3):151–158.
Johnson, T. “Homelessness and Drug Use,” American Journal of Preventive Medicine, no. 32, Issue 6,
2007.
Krentzman AR, Robinson EA, Moore BC, Kelly JF, Laudet AB, White WL, Strobbe S. How
Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) work: Cross-disciplinary perspectives.
Alcohol Treatment Quarterly. 2010;29(1):75–84.
Lyons, G. C., Deane, F. P., & Kelly, P. J. (2010). Forgiveness and purpose in life as spiritual mechanisms
of recovery from substance use disorders. Addiction Research & Theory, 18(5), 528-543.
Mattick et al., Methadone Maintenance Therapy Versus No Opioid Replacement Therapy for Opioid
Dependence. Cochrane Database of Systematic Reviews, 3, (2009).
McCarty, D., Braude, L., Lyman, D. R., Dougherty, R. H., Daniels, A. S., Ghose, S. S., &
Delphin-Rittmon, M. E. (2014). Substance abuse intensive outpatient programs: Assessing the
evidence. Psychiatric Services, 65(6), 718–726.
McKellar J, Stewart E, Humphreys K. Alcoholics Anonymous involvement and positive alcohol-related
outcomes: Consequence, or just a correlate? A prospective 2-year study of 2,319 alcohol-dependent
men. Journal of Consulting and Clinical Psychology. 2003;71(2):302–308.
Moos RH, Moos BS. Participation in treatment and alcoholics anonymous: A 16-year follow-up of
initially untreated individuals. Journal of Clinical Psychology. 2006;62(6):735–750.
(n.d.). 5 Ways Spirituality Boosts Addiction Recovery. Ashley Treatment. Retrieved December 21, 2022,
from https://www.ashleytreatment.org/5-ways-spirituality-boosts-recovery/
Owen PL, Slaymaker V, Tonigan JS, McCrady BS, Epstein EE, Kaskutas LA, Miller WR. Participation
in alcoholics anonymous: Intended and unintended change mechanisms. Alcoholism: Clinical and
Experimental Research. 2003;27(3):524–532.
Samet J H, Friedmann P D, Saitz R. “Benefits of Linking Primary Medical Care and Substance Abuse
Services: Patient, Provider, and Societal Perspectives.” Archives of Internal Medicine.
2001;161(1):85–91.
Samet J H, Saitz R, Larson M J. “A Case for Enhanced Linkage of Substance Abusers to Primary
Medical Care.” Substance Abuse. 1996;17(4):181–92.
Center for Substance Abuse Treatment. Substance Abuse: Clinical Issues in Intensive Outpatient
Treatment. Rockville (MD): Substance Abuse and Mental Health Services Administration (US); 2006.
(Treatment Improvement Protocol (TIP) Series, No. 47.) Chapter 4. Services in Intensive Outpatient
Treatment Programs. Available from: https://www.ncbi.nlm.nih.gov/books/NBK64094/
Sinha, R. “Chronic Stress, Drug Use, and Vulnerability to Addiction,” Annals of the New York
Academy of Sciences, July 2018.
Smith, M. A., & Lynch, W. J. (2012). Exercise as a potential treatment for drug abuse: evidence from
preclinical studies. Frontiers in psychiatry, 2, 82.
Specter, S. E., & Wiss, D. A. (2014). Muscle dysmorphia: Where body image obsession, compulsive
exercise, disordered eating, and substance abuse intersect in susceptible males. In Eating disorders,
addictions and substance use disorders (pp. 439-457). Springer, Berlin, Heidelberg.
Weiss RD, Griffin ML, Gallop RJ, Najavits LM, Frank A, Crits-Christoph P, Luborsky L. The effect of
12-step self-help group attendance and participation on drug use outcomes among cocaine-dependent
patients. Drug and Alcohol Dependence. 2005;77(2):177–184.
White, W. L. (2009). Peer-Based Addiction Recovery Support: History, Theory, Practice, and Scientific
Evaluation Executive Summary. Counselor., 10(5), 54-59.
Ziguras, S., & Stuart, G. W. (2000). A meta-analysis of the effectiveness of mental health case
management over 20 years. Psychiatric Services, 51, 1410–1421.
Appendix – Weekly Survey
- Approximately how many minutes did you spend talking to your case manager this week?
a. None
b. 15
c. 30
d. 45
e. 60
f. More than 60 - How many hours did you spend working in a legal job last week? (If you didn’t work last week,
put zero.)
a. 0
b. 1-10
c. 11-20
d. 21-30
e. 31-40
f. More than 40 - What is your hourly wage?
- What is your current housing situation?
a. Homeless
b. Shelter
c. Transitional Living
d. Supervised Half-way house
e. Sober / Recovery Living
f. Independent Living - In the past week, how many hours did you spend working on your spirituality / getting closer
to your higher power?
a. 0
b. 1
c. 2
d. 3-4
e. 5-6
f. 7 or more - How many recovery meetings (e.g., AA, NA) did you attend in the past week?
- In the past week, how many one-on-one peer recovery sessions did you attend?
- Which of the following salon services did you receive in the past week?
a. Haircut
b. Manicure
c. Pedicure
d. None
e. Other ____________ - How many hours in the past week did you engage in any physical fitness?
a. 0
b. 1
c. 2
d. 3-4
e. 5-6
f. 7 or more - In the past week, how many hours did you spend in service to others?
a. 0
b. 1
c. 2
d. 3-4
e. 5-6
f. 7 or more

